Spinal osteochondrosis is a degenerative disease of the spine (that is, associated with the gradual destruction of tissue and disruption of its function).The main changes are associated with the intervertebral disc (elastic formation located between the vertebrae and which is a type of shock absorber that softens the shocks and vibrations of the vertebrae in relation to each other when walking).With osteochondrosis, the intervertebral discs become calloused, harden and often protrude into the spinal canal, where they can compress the spinal cord itself or its roots, causing corresponding complaints (pain in the arms and legs, back, numbness of the skin of the extremities).
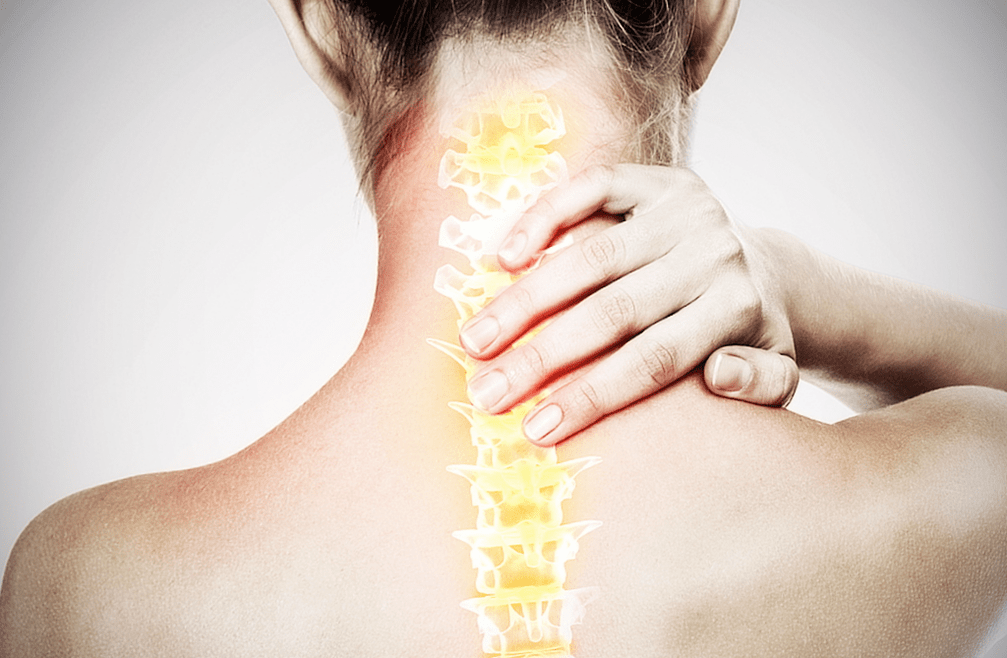
Spinal osteochondrosis symptoms
- Back and neck pain: especially at night, after physical activity.
- Sensation of painful tension in individual back muscles.
- Numbness of the skin on the arms or legs (fingertips or as a separate band on the skin).
- Weakness in the muscles of the arms or legs.
- Atrophy (thinning) of the muscles in the arms and legs.
- Dizziness, headaches: when the vertebral artery that supplies the brain is compressed between the cervical vertebrae.
Forms
- Depending on which part of the spine the greatest changes are located, the following forms of spinal osteochondrosis are distinguished:
- osteochondrosis of the cervical spine;
- osteochondrosis of the thoracic spine;
- osteochondrosis of the lumbar spine.
- Depending on the structural changes that have occurred in the intervertebral disc (elastic formation located between the vertebrae), the following stages of spinal osteochondrosis are distinguished:
- Stage 1: intradiscal movement of the disc nucleus (dense formation in its center) towards the edge;
- Stage 2: appearance of fissures in the fibrous ring of the disc (made up of connective tissue) and instability of the spine (excessive mobility);
- Stage 3: complete rupture of the disc with its prolapse in the form of a hernia into the spinal canal, possible compression of the spinal cord roots;
- Stage 4: gross changes not only in the intervertebral discs, but also in the surrounding tissues (excessive growth of bone tissue, strong pathological attachment of the vertebrae to each other).
Reasons
- Excessive stress on the spine:
- occupational risks: heavy lifting (e.g. for loaders), prolonged work in a static (immobile) position;
- excess body weight, which increases the load on the spine;
- lifting excessively large (exorbitantly heavy) objects.
- Spinal injuries: vertebral fractures, ligament ruptures.
- Hereditary causes: tendency to gradual disruption of nutrition of the vertebrae and the tissues surrounding them (ligaments, intervertebral discs).
Diagnosis
- Analysis of complaints and medical history:
- How long ago did you first experience back pain, numbness in your fingers and toes, and other complaints?
- whether professional or domestic activities are associated with lifting heavy objects, maintaining a motionless position of the back and neck for a long time (sitting at a table, etc.).
- Neurological examination: search for signs of neurological disorders (impaired sensitivity in the arms or legs, curvature of the spine, pain when palpating the muscles of the back and neck).
- Spine radiography: this method allows you to study the structure of the spine in one or more planes, detect thinning of the intervertebral discs (elastic formation located between the vertebrae), their protrusion towards the spinal canal, as well as marginal growth of the bone tissue of the spine (osteophytes), which are also a consequence of malnutrition of the spine and can damage the spinal roots, causing pain and sensitivity disorders.
- CT (computed tomography) and magnetic resonance imaging (magnetic resonance imaging) of the spine in the cervical and spinal regions: allow layer-by-layer study of the structure of the spine and surrounding tissues (intervertebral discs, ligaments) and detect thinning of the intervertebral discs, the presence and size of protrusion (hernia) of the discs in the space between the vertebrae.
Treatment of spinal osteochondrosis
- Limit the load on the spine (do not lift heavy objects).
- Proper distribution of load on the spine: for example, carry bags not in one hand, but in both, which makes the load more uniform.
- Massage on the back and neck area.
- Physiotherapy: set of exercises that strengthen the spinal muscles.
- Swimming.
- Acupuncture: influencing the local processes of destruction of intervertebral disc tissue through injections with special small needles.
- Painkillers.
- Medicines that reduce muscle tension (muscle relaxants).
- For advanced processes (hernia prolapse with compression of the roots of the spinal cord), surgical treatment (removal of the intervertebral disc, fixation of the affected part of the spine).
Complications and consequences
- Chronic back pain.
- Paralysis (weakness in the arms or legs).
- Poor cerebral circulation (when the vertebral artery that supplies the brain is compressed between the cervical vertebrae).
Spinal osteochondrosis prevention
- Gentle work regime: moderate lifting of weight, refusal to lift excessively heavy objects, periodic changes in physical and mental work (to “stretch” the spine).
- Active recreation.
- Gymnastics, morning exercises: daily performing simple exercises that involve the spine (trunk turns, light push-ups).

























